Kunming, China, June 21, 2023
KBI has established a step-wise screening system with the use of clinical chemistry, blood biomarkers, echocardiogram and myocardial MRI to characterize different types
of heart failure (HF) with a large body of database. We have produced models of heart failure with either reduced ejection fraction (HFrEF, or systolic failure) or preserved
ejection fraction (HFpEF, diastolic failure) from more than 1,000 prolonged HFD monkeys (Fig 1).
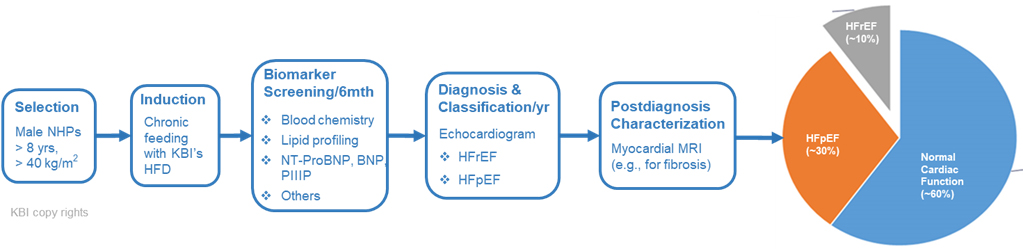
Fig 1. Induction, step-wise screening and characterization of metabolic heart failure in monkeys at KBI.
Typically, about 40% of these monkeys develop different extents of heart failure with typical pathological features after two years of chronic HFD (Fig 2). These monkeys
have been classified into systolic (HFrEF) or diastolic (HFpEF) heart failures (Fig 3) and successfully used for a series of studies to test new drugs.
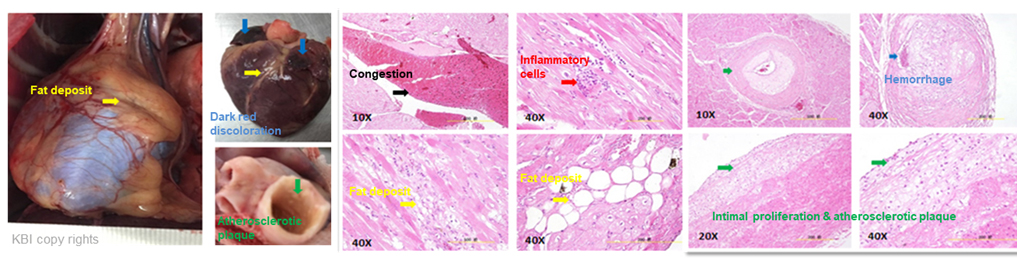
Fig 2. Representative pathology features in monkeys with metabolic heart failure induced by chronic HFD.
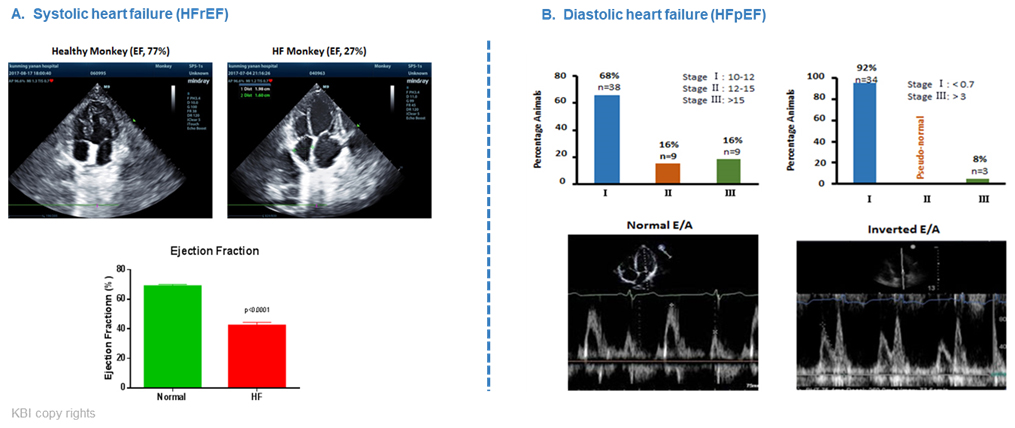
Fig 3. Two types of metabolic heart failure in NHPs characterized at KBI. A. Systolic (HFrEF) and B Diastolic (HFpEF) dysfunction.
N-terminal pro-brain natriuretic peptide (NT-proBNP) is a specific biomarker used for the assessment of the progression and treatment responses in patients with chronic
heart failure (CHF). As shown in Fig 4, NT-proBNP is significantly elevated in the CHF monkeys and KBI has used this biomarker to assess efficacy of test drugs.
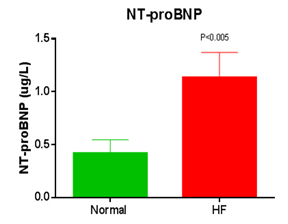
Fig 4. NT-proBNP is increased in monkeys with metabolic heart failure.
Furthermore, KBI has in-house myocardial MRI in place for the evaluation of interstitial cardiac fibrosis and left ventricular ejection fraction (LVEF). MRI T1 mapping for
determination of extracellular matrix volume (ECV) as a surrogate is a powerful diagnostic tool for detailed evaluation of heart failure in patients. As exemplified in
Fig 5, the myocardial MRI results obtained at KBI monkeys with heart failure closely resemble the reported characteristics in patients under similar conditions.
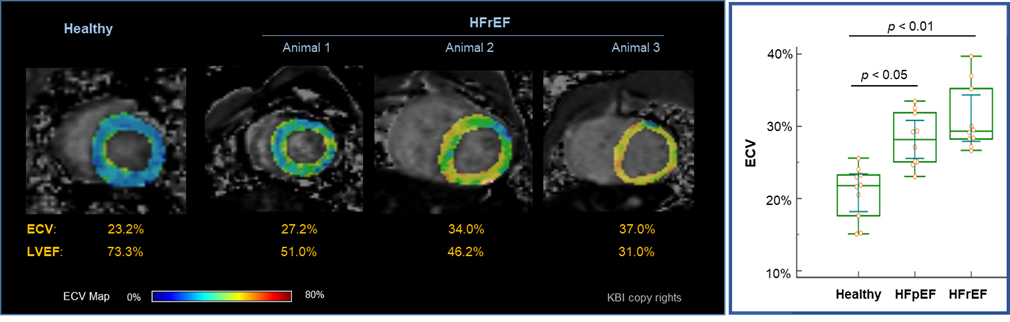
Fig 5. MRI T1 ECV as a surrogate for evaluation of myocardial fibrosis in monkeys with metabolic heart failure induced by chronic HFD.
Contact us if you need more information.